Fentanyl and Methamphetamine in South Jersey: The Evolving Substance Landscape

One of the most alarming trends in New Jersey is the rampant spread of illicit fentanyl and its methamphetamine in South Jersey. According to a DEA report, in early 2025, fentanyl and norfentanyl appeared in nearly 40% of all drug-positive tests, underscoring fentanyl’s dominant and lethal influence in the state’s drug supply. Moreover, adulterants like xylazine—a veterinary tranquilizer—now contaminate many opioid mixtures, which complicates overdose responses since xylazine does not respond to naloxone. In combination, these hidden substances dramatically increase overdose risk and pose new challenges for first responders and treatment providers across South Jersey. Equally concerning is the resurgence of methamphetamine use. Once relatively scarce in the region, meth is becoming more accessible—and increasingly laced with fentanyl—in rural and suburban areas. New Jersey’s “fourth wave” of substance abuse includes rising rates of stimulant-related deaths. Nationally, overdose fatalities involving stimulants like methamphetamine have surged more than 300% since 2015, a pattern that’s echoed locally in South Jersey. This complex, polysubstance threat demands integrated treatment protocols targeting stimulant, opioid, and tranquilizer misuse together. Overdose Rates & Demographic Shifts Recent data from the New Jersey Medicolegal Death Review System shows that, between January and April 2025, Ocean County and other southern Jersey counties recorded over 12 suspected overdose deaths monthly, similar to 2024’s figures of ~171 for the full year. In neighboring Camden County, suspected overdose deaths surged to 327 in 2023, making it one of the hardest-hit areas in the state. Despite statewide declines—New Jersey reported 2,778 overdose deaths in 2023, down from 3,047 in 2021—certain counties continue to bear a disproportionate burden. Demographics also reveal critical trends: 2024 data indicate more than 65% of overdose victims were male, and adults aged 35–44 represented the highest age-group prevalence. However, younger adults, particularly those aged 25–34, are increasingly affected by polysubstance overdoses involving fentanyl and stimulants. Another notable shift: overdose deaths among Black and Hispanic residents, particularly older adults, are rising—a sign that equity-focused interventions are urgently needed. Treatment Admissions and Service Gaps New Jersey reported 98,479 hospital admissions for substance use in 2024, indicating widespread demand for treatment. Of these, nearly 20% (≈approximately 19,000) were for outpatient care, while around 17,000 individuals received Intensive Outpatient Program (IOP) services, underscoring the importance of flexible, community-based care. Notably, alcohol and heroin remain the most common substances driving treatment entries, accounting for 40.5% and 31% of admissions, respectively. Despite these treatment efforts, only about 7–10% of facilities in southern New Jersey offer integrated care for co-occurring disorders—a troubling figure given the prevalence of mental health issues in addiction. Additionally, treatment deserts persist in rural areas, and many patients can’t access care promptly, delays that increase the risk of relapse or overdose. Fortunately, New Jersey’s increased funding (e.g., opioid lawsuit settlement) is improving infrastructure and access, though persistent gaps remain. Prevention, Harm Reduction, and Policy Responses In response to this evolving crisis, New Jersey has implemented several public health initiatives to curb overdose deaths. Key strategies include widespread naloxone distribution, enforceable by law as of 2021, and lagging but increasing availability of fentanyl test strips. EMS and first responders in South Jersey are trained to carry multiple doses due to the potency of fentanyl/Xylazine mixtures. Local agencies also launched drug awareness programs targeting youth to address the rising prevalence of stimulant and opioid use among teens and young adults. Legislative action includes tighter prescription monitoring and zoning laws to regulate treatment centers, striking a balance between accessibility and community protection. The deployment of opioid settlement revenues (~$600M statewide) is funding sustainable recovery services, expanded treatment access, and post-treatment support. The Path Forward for South Jersey The shifting landscape of addiction in South Jersey—driven by fentanyl dominance, returning meth use, and poly-drug trends—demands a multi-pronged response. Integrated treatment that addresses multiple substance use and mental health disorders, harm reduction, and community-based prevention must all be strengthened. Data indicate that county-level variation remains wide, underscoring the need for regionally tailored interventions. For individuals and families seeking help, awareness of outpatient IOPs and comprehensive dual-diagnosis clinics is key. As policies and funding shift toward community-based models, South Jersey must also ensure access in underserved areas—rural, suburban, and urban alike. Community engagement, educational campaigns, and peer-led support will be essential complements to clinical care. Ready to Take the Next Step Towards Recovery? If you’re in South Jersey and looking for support, the team at Avisa Recovery in Toms River, NJ offers specialized, evidence-based treatment tailored to meet the challenges of today’s complex addiction trends. From integrated outpatient programs to individualized care that includes trauma-informed and holistic therapies, we are here to guide you every step of the way. Contact Avisa Recovery today to schedule a confidential assessment and discover how our services can help you navigate these evolving addiction challenges—and reclaim your health and hope.
Am I an Alcoholic?

Alcohol is a widely accepted part of social life, but when drinking begins to interfere with your well-being, you might find yourself asking, “Am I an alcoholic?” It’s a question that many people face at some point, especially if alcohol use starts to impact relationships, work, or physical and mental health. At Avisa Recovery, we help individuals across Monmouth County find answers, clarity, and a path to recovery. If you’re wondering whether your drinking habits are regular or a sign of something deeper, this guide breaks down the signs of alcoholism, what it means to struggle with alcohol use disorder (AUD), and how you can take the first step toward lasting change. What Does It Mean to Be an Alcoholic? The term “alcoholic” is often misunderstood. It doesn’t always mean someone who drinks all day or hits rock bottom before seeking help. Many people with alcohol use disorder function in their daily lives, maintaining jobs and relationships, yet still struggle privately with their drinking. Alcoholism, or alcohol use disorder (AUD), is a medical condition characterized by an impaired ability to stop or control alcohol use despite adverse consequences. The severity can range from mild to severe, and the earlier it’s addressed, the better the chances of successful recovery. Am I an Alcoholic? Key Signs to Look For Asking yourself, “Am I an alcoholic?” is an important first step, but recognizing the signs can bring you closer to the truth. Here are some red flags to consider: You Can’t Stop After One or Two Drinks If you often plan to have “just one” and end up drinking more than intended, it may be a sign of a deeper issue. Loss of control over drinking is a common trait in people with AUD. You Drink to Cope with Stress or Emotions Do you reach for alcohol when you’re sad, anxious, angry, or overwhelmed? Using alcohol as an emotional escape can create a dependency that grows stronger over time. You Experience Withdrawal Symptoms Shaking, sweating, irritability, insomnia, or nausea after stopping alcohol may point to physical dependence. This is a critical indicator that your body has adapted to alcohol and reacts negatively when it’s absent. You’ve Tried to Quit But Couldn’t Many people who struggle with alcohol try to cut back or stop on their own. If you’ve made several attempts to quit but always go back to drinking, you might benefit from professional help. Drinking Is Hurting Your Relationships or Responsibilities Have loved ones expressed concern? Have you missed work or neglected essential duties because of alcohol? These are clear signs that alcohol may be taking over parts of your life. You Hide or Downplay Your Drinking If you lie about how much you drink or feel the need to hide it, it’s worth examining why. Shame and secrecy often go hand-in-hand with addiction. The Difference Between Problem Drinking and Alcoholism It’s possible to engage in problematic drinking without having full-blown alcohol use disorder, but that doesn’t mean it should be ignored. Problem drinking is a slippery slope, and without intervention, it can quickly progress. Here’s how the two differ: Problem Drinking: Drinking in ways that cause issues in your life, but haven’t resulted in physical dependence. Alcohol Use Disorder (AUD): A chronic disease involving an inability to control drinking, strong cravings, and physical withdrawal symptoms. Either way, if alcohol is causing harm, seeking help is a proactive, courageous step, not a weakness. Why It’s So Hard to Admit There’s a Problem Many people resist the idea of being labeled an “alcoholic” because of stigma, shame, or fear of change. But asking “Am I an alcoholic?” is a decisive moment of self-awareness. Denial is one of the most common barriers to treatment—yet facing the issue head-on is often the turning point toward a better life. Remember, alcoholism doesn’t look the same for everyone. You don’t need to hit rock bottom to get help. If drinking is making your life harder in any way, you deserve support. How Avisa Recovery Can Help At Avisa Recovery, we specialize in helping individuals in Monmouth County find freedom from alcohol addiction through compassionate, evidence-based care. We offer: Medical detox to safely manage withdrawal symptoms Individual and group therapy to address the root causes of addiction Dual diagnosis treatment for co-occurring mental health conditions Holistic services such as mindfulness, fitness, and nutrition support Flexible care options, including outpatient and intensive outpatient programs We understand that no two recovery journeys are alike, which is why our team tailors treatment to your unique needs and goals. Whether you’re just beginning to question your relationship with alcohol or are ready to commit to sobriety, we’ll meet you where you are—judgment-free. Take the First Step Toward a Healthier Life If you’re still asking yourself, “Am I an alcoholic?”—it might be time to talk to someone who can help you sort through the uncertainty. You don’t have to navigate this alone. Contact Avisa Recovery today to learn more about our trusted alcohol rehab in Monmouth County. Our team is here to support your healing, one step at a time. Let us help you rediscover life without alcohol.
Is There Such a Thing as Taking Too Many Psych Meds?

In today’s world, mental health awareness is more prominent than ever. With growing recognition comes greater access to treatment options, including psychiatric medications. While many can benefit from psych meds, some may question if they are taking too many psych meds. Antidepressants, anti-anxiety drugs, mood stabilizers, and antipsychotics have helped millions of people manage mental health conditions like depression, anxiety, bipolar disorder, and schizophrenia. But as prescriptions become more common, some people are left wondering: Is there such a thing as taking too many psych meds? At Avisa Recovery of New Jersey, we believe in a balanced, individualized approach to mental health care. While psychiatric medication can be life-changing and even life-saving, overmedication is a genuine concern. Understanding the risks, signs, and available solutions is crucial for selecting the most effective treatment path. When Medication Becomes Too Much Psychiatric medications can be powerful tools, but they aren’t a one-size-fits-all solution. It’s possible—and surprisingly common—for individuals to end up on multiple prescriptions at once. This is known as polypharmacy, and while it can be appropriate in some cases, it also carries potential risks if not carefully monitored. Overmedication may occur due to: Misdiagnosis or overlapping conditions Medication side effects are being mistaken for new symptoms A lack of coordination between different prescribing doctors Long-term reliance on medications without regular re-evaluation Taking too many psych meds can lead to unwanted side effects, reduced effectiveness, and a loss of connection to your authentic self. It’s not about eliminating medication altogether, but rather finding the right combination and dosage for your unique needs. Signs You May Be Taking Too Many Psych Meds It’s not always easy to recognize when psychiatric medication has gone too far. Some individuals live for years with symptoms that could be related to overmedication without ever realizing it. Here are common warning signs that may suggest you’re taking too many psych meds: Emotional flatness or numbness: You may find it difficult to feel joy, sadness, or motivation. While some medications reduce intense emotional swings, they shouldn’t eliminate emotion altogether. Mental fog or memory issues: Trouble concentrating, forgetfulness, or disorientation can result from too much medication or an improper combination. Excessive drowsiness or sedation: Feeling chronically fatigued or unable to function during the day may signal that your dosages are too high. Physical side effects: Tremors, weight gain, gastrointestinal issues, and other side effects may become more intense with multiple medications. Mood instability: Ironically, the wrong medication mix can cause the very symptoms it’s meant to treat, such as increased anxiety, depression, or irritability. If you notice any of these symptoms, don’t stop your medication abruptly. Instead, reach out to a qualified mental health professional who can guide you through a safe evaluation process. Why Overmedication Happens It’s easy to assume that more medication equals more relief, but that’s not always true. Over time, people may receive new prescriptions to address side effects, resulting in a cycle where new drugs are added rather than carefully adjusted. In these instances, you may be taking too many psych meds. Other factors that contribute to overmedication include: Fragmented care: Multiple doctors prescribing medications without consulting each other can lead to unintentional polypharmacy. Trial and error: It often takes time to find the proper medication or dosage. Without apparent oversight, this can spiral into unnecessary combinations. Short appointments: In busy systems, providers may prescribe medications quickly without exploring other options, such as therapy or lifestyle changes. Pressure to feel “better fast”: To ease suffering quickly, there’s sometimes an over-reliance on medication before addressing underlying causes. At Avisa Recovery, we understand how complex this process can be. That’s why we take the time to assess the whole picture—your symptoms, history, and lifestyle—before making any recommendations. Finding the Right Balance Psych meds can offer incredible benefits when used appropriately. They can reduce symptoms, stabilize mood, and enhance the effectiveness of therapy. The key is balance. Medication should improve your life, not dull it. To avoid taking too many psych meds, it’s important to: Work with a comprehensive treatment team That Includes Psychiatrists, therapists, and primary care providers who collaborate regularly. Schedule regular medication reviews: Your treatment plan should be re-evaluated at least every few months to determine what’s working and what’s not. Explore holistic support options: Therapy, nutrition, exercise, mindfulness, and other wellness strategies can reduce the need for multiple prescriptions. Advocate for yourself: If something feels off, speak up. You know your body and mind better than anyone. At Avisa Recovery, we support clients in making informed decisions about medication. We’ll never suggest stopping necessary prescriptions, but we’ll help you understand what you’re taking, why, and whether there’s a better way to support your mental health. When to Re-Evaluate Your Medication Plan If you’ve been on multiple psych meds for an extended period or if you feel disconnected from yourself, it may be time for a medication assessment. This doesn’t mean stopping cold turkey. Instead, it involves a guided, medically supervised process to evaluate the role of each medication in your treatment. In some cases, simplifying your regimen can enhance mental clarity, minimize side effects, and even foster a stronger emotional connection. In other cases, adjusting dosages or adding therapy may be the key to sustainable progress. Take the Next Step Toward Mental Wellness Yes, there is such a thing as taking too many psych meds—but you don’t have to figure it out alone. Whether you’re questioning your current medication plan or starting your mental health journey for the first time, we’re here to help. Contact Avisa Recovery of New Jersey today to learn more about our comprehensive mental health treatment options. Our compassionate team will work with you to find the right balance between therapy, medication, and holistic care, so you can feel like yourself
Veterans & PTSD: The Need For Immediate Care

Veterans and PTSD are often spoken about in the same breath, and for good reason. Many of our nation’s heroes return home with deep psychological wounds that are less visible than physical injuries but just as devastating. For veterans, the impact of trauma can be long-lasting, and the need for immediate mental health care is critical. At Avisa Recovery of New Jersey, we recognize the urgent need for specialized support and treatment designed specifically for veterans living with PTSD. Post-Traumatic Stress Disorder (PTSD) affects a significant percentage of veterans, often as a result of experiencing or witnessing life-threatening events during military service. Combat exposure, traumatic injuries, sexual assault, and prolonged stress can all contribute to the development of PTSD. Without timely and effective care, this condition can interfere with every aspect of a veteran’s life, including relationships, career, and physical health. Why Veterans and PTSD Require Immediate Attention The connection between veterans and PTSD is not just a topic of awareness—it’s a matter of public health. According to the U.S. Department of Veterans Affairs, anywhere from 11% to 30% of veterans suffer from PTSD, depending on the conflict in which they served. Yet, many go undiagnosed or untreated for years. Delaying treatment often worsens the condition. Veterans with untreated PTSD may experience: Chronic anxiety and panic attacks Flashbacks and nightmares Hypervigilance and emotional numbness Irritability, depression, and suicidal thoughts Substance abuse as a coping mechanism The longer PTSD is left unaddressed, the more it disrupts a veteran’s ability to function and thrive. That’s why early intervention is not only necessary—it’s essential for recovery and quality of life. Barriers Veterans Face in Getting Help Even though the link between veterans and PTSD is well-documented, many service members still hesitate to seek treatment. There are several reasons for this: Stigma: Some veterans fear that asking for mental health support will be seen as a sign of weakness, especially in military culture. Lack of access: While the VA offers resources, the system can be overburdened, slow, or difficult to navigate. Fear of losing benefits or career opportunities: Veterans worry that a mental health diagnosis might impact their job prospects or security clearances. Emotional avoidance: Reliving trauma can be painful, and the idea of revisiting those experiences in therapy can feel overwhelming. These barriers make it even more important to provide safe, accessible, and veteran-friendly mental health services that emphasize trust, dignity, and healing. How PTSD Affects Daily Life for Veterans Veterans with PTSD often face unique challenges when reintegrating into civilian life. The symptoms of PTSD can interfere with daily functioning, affecting everything from employment to family life. Relationships: Veterans may struggle with intimacy, communication, or emotional regulation, which puts strain on marriages and parenting. Workplace challenges, such as concentration problems, sleep disturbances, or anxiety, can hinder job performance or lead to unemployment. Health concerns: PTSD is closely linked to physical health issues, including chronic pain, gastrointestinal problems, and increased risk of heart disease. Isolation: Many veterans feel disconnected from those who haven’t shared their experiences, leading to withdrawal and loneliness. These struggles are not a reflection of personal weakness—they’re the result of unprocessed trauma. And they are treatable with the right approach. Why Avisa Recovery Is the Right Place for Veterans At Avisa Recovery of New Jersey, we offer compassionate, evidence-based care tailored to the needs of veterans. We understand the complexities of PTSD and the cultural nuances of military life. Our veteran-focused treatment programs provide: Trauma-informed therapy: Including EMDR (Eye Movement Desensitization and Reprocessing), cognitive behavioral therapy (CBT), and prolonged exposure therapy. Dual diagnosis treatment: For veterans managing both PTSD and substance use or co-occurring mental health disorders. Individualized care plans: Developed with input from clinical experts who understand military trauma. Group therapy with other veterans: Group therapy can help reduce isolation and build peer support. Family involvement: Because healing often requires the support and understanding of loved ones. Our goal is to create a safe, structured space where veterans can explore their trauma, rebuild their confidence, and move toward lasting recovery. Veterans and PTSD: It’s Time to Prioritize Mental Health Veterans and PTSD should never be an afterthought. These are individuals who have sacrificed their time, health, and well-being in service of our country, and they deserve immediate, high-quality care when they return home. While there is no single cure for PTSD, there are effective, proven treatments that can help veterans reclaim their lives. If you or a loved one is a veteran struggling with PTSD, now is the time to act. Early intervention saves lives, strengthens families, and restores hope. Contact Avisa Recovery of New Jersey today to learn more about our specialized mental health treatment programs for veterans. Our team is ready to help you find the peace and healing you deserve. Let us stand by your side on the journey to recovery.
Should You Go to a Psychiatrist?

If you’ve ever found yourself wondering, “Should I go to a psychiatrist?”—you’re not alone. Mental health is just as important as physical health, yet many people hesitate to seek help when they’re struggling emotionally or mentally. At Avisa Recovery of New Jersey, we believe that reaching out for psychiatric support is a powerful and brave step toward healing. So, should you go to a Psychiatrist? We help answer this question. Whether you’re experiencing symptoms for the first time or you’re looking for better ways to manage ongoing challenges, seeing a psychiatrist might be precisely what you need. Psychiatrists are medical doctors who specialize in diagnosing, treating, and managing mental health disorders. Unlike therapists or psychologists, psychiatrists can prescribe medication and offer a medical perspective on your emotional and psychological symptoms. Their expertise can be life-changing for individuals dealing with depression, anxiety, bipolar disorder, PTSD, or other mental health conditions that benefit from clinical evaluation and medication management. When Should You Go to a Psychiatrist? So, how do you know when it’s time to talk to a psychiatrist? The truth is, there’s no one-size-fits-all answer. But several signs and situations suggest it might be the right move. You’re Struggling with Daily Functioning If your mental health symptoms are interfering with your ability to function—whether that’s at work, in relationships, or with daily responsibilities—it may be time to seek professional help. Psychiatrists are trained to assess how mental health conditions affect your life and can develop a personalized treatment plan to improve your well-being. You’ve Tried Therapy Alone but Need More Therapy can be incredibly effective, but sometimes it’s not enough on its own. If you’ve been working with a therapist and your symptoms haven’t improved—or have worsened—a psychiatrist can evaluate whether medication might help. Many people benefit most from a combination of therapy and psychiatric care. You’re Experiencing Severe Symptoms Certain symptoms may indicate the need for immediate psychiatric evaluation, such as: Persistent feelings of sadness or hopelessness Frequent panic attacks or extreme anxiety Unexplained mood swings Thoughts of self-harm or suicide Difficulty sleeping, eating, or concentrating Hallucinations or delusions These symptoms may point to an underlying mental health condition that requires medical attention. You Have a Family History of Mental Health Conditions If mental illness runs in your family, you may have a higher risk of developing a similar condition. A psychiatrist can provide early screenings, monitor symptoms, and recommend preventative strategies or treatments if needed. What to Expect at a Psychiatrist Appointment Taking the step to see a psychiatrist may feel intimidating, especially if you’ve never been before. But understanding what to expect can ease your concerns. During your first appointment, your psychiatrist will: Ask about your current symptoms, thoughts, behaviors, and emotions Discuss your personal and family medical history Review any medications you’re currently taking Conduct a mental status examination Begin to formulate a diagnosis and treatment plan This is a collaborative process. The psychiatrist will listen to your concerns and help you make informed decisions about next steps. Treatment may include medication, therapy referrals, or lifestyle recommendations. The Role of Medication in Mental Health Treatment One of the most common reasons people visit a psychiatrist is for medication management. Psychiatric medications—such as antidepressants, mood stabilizers, and anti-anxiety drugs—can help correct chemical imbalances in the brain that contribute to mental health symptoms. But medication isn’t a magic fix. It’s most effective when it’s carefully monitored and adjusted as needed. That’s why working with a psychiatrist who understands your unique needs is so important. They’ll track your progress, watch for side effects, and ensure the medication continues to support your recovery. At Avisa Recovery, our psychiatrists take a thoughtful, individualized approach to medication management. We don’t just hand out prescriptions—we take the time to get to know you, your challenges, and your goals. Breaking the Stigma One of the most significant barriers to seeking psychiatric help is stigma. Many people fear being judged or labeled as “crazy” for seeing a psychiatrist. But here’s the truth: asking for help is a sign of strength, not weakness. Just as you would visit a doctor for high blood pressure or diabetes, it’s normal and healthy to see a psychiatrist for emotional or mental concerns. Your mental health matters, and getting the proper care can dramatically improve your quality of life. Should You Go to a Psychiatrist? The Answer Might Be Yes If you’re still asking yourself, “Should I go to a psychiatrist?”—that question alone is a good reason to explore the option. You don’t have to be in crisis to benefit from psychiatric support. Early intervention can prevent more serious issues down the road and help you feel more stable, focused, and empowered. At Avisa Recovery of New Jersey, we’re here to support you with compassionate, expert psychiatric care and medication management. Whether you’re navigating a recent diagnosis or have been managing symptoms for years, we’re ready to walk beside you every step of the way. Contact Avisa Recovery today to learn more about our comprehensive psychiatric services and medication management options in New Jersey. Your mental health journey deserves attention, and we’re here to help you thrive.
How to Get Medication for Depression: A Step-by-Step Guide
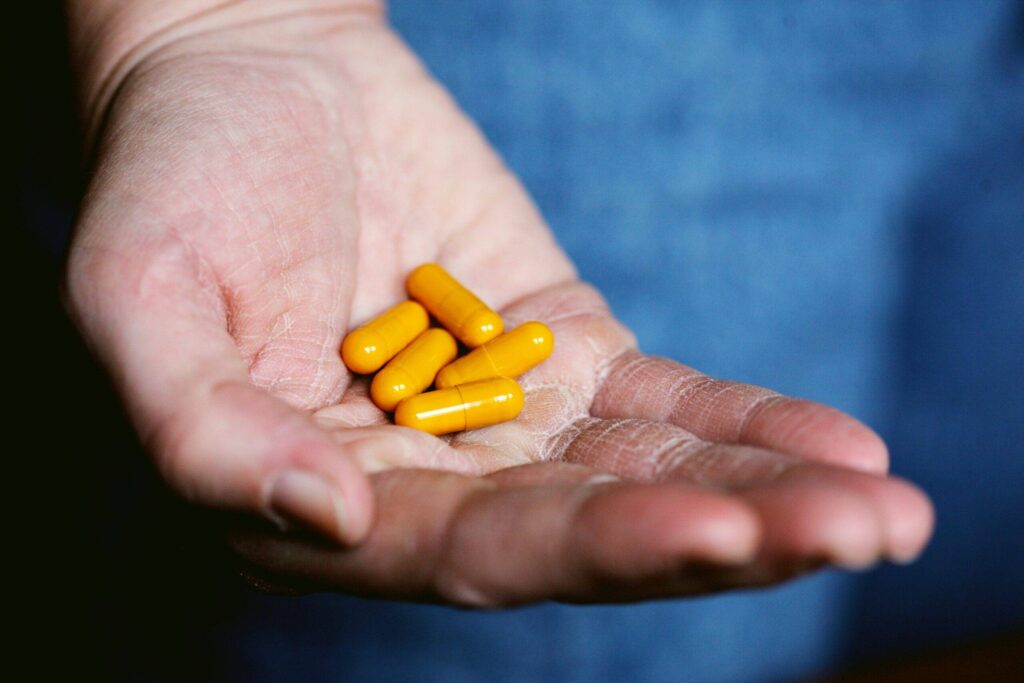
If you’re struggling with persistent sadness, low energy, or loss of interest in daily life, you may be wondering how to get medication for depression. This form of treatment can be a powerful tool in managing symptoms and restoring emotional balance, especially when combined with therapy and other supportive approaches. At Avisa Recovery, we understand the challenges of living with depression and are here to help you navigate the process of accessing the care you need. Recognizing When You Might Need Medication for Depression Before starting medication for depression, it’s important to recognize the signs that treatment might be necessary. Depression presents differently in everyone, but common symptoms include: Persistent sadness or hopelessness Loss of interest in previously enjoyed activities Changes in sleep or appetite Trouble concentrating or making decisions Fatigue or lack of motivation Thoughts of self-harm or suicide If these symptoms have lasted for two weeks or more and are interfering with your ability to function, it may be time to explore your treatment options. Documenting your experiences can help a healthcare provider determine whether depression medication could be beneficial. How to Speak to a Professional About Medication for Depression The first step in obtaining medication for depression is scheduling an appointment with a medical or mental health professional. Several types of providers can assess your symptoms and prescribe treatment: Primary Care Providers – General practitioners can evaluate your symptoms and often initiate a prescription for depression medication. Psychiatrists – These mental health specialists focus exclusively on psychiatric conditions and can offer more tailored treatment plans. Nurse Practitioners or Physician Assistants – These professionals, especially those working in mental health settings, are also qualified to prescribe antidepressants. Be open and honest during your appointment. Describe how your symptoms affect your daily life, relationships, and school or work performance. This transparency helps ensure the right diagnosis and the most effective treatment plan. Types of Medication for Depression There are various medications for depression options, and your provider will help determine which is most appropriate based on your specific needs. Common classes include: Selective Serotonin Reuptake Inhibitors (SSRIs) – Often the first type prescribed, including medications like Prozac, Zoloft, and Lexapro. Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs) – Such as Cymbalta and Effexor, which affect multiple neurotransmitters to alleviate symptoms. Atypical Antidepressants – Like Wellbutrin, these can be beneficial for individuals who don’t respond well to SSRIs or SNRIs. It can take several weeks to notice the full effects of depression medication, and some people may need to try more than one type before finding the right fit. Your provider may adjust your dose or switch medications as needed. Combining Medication for Depression with Other Treatments While medication for depression can significantly reduce symptoms, it is often most effective when paired with other forms of treatment. Cognitive Behavioral Therapy (CBT), Dialectical Behavior Therapy (DBT), and mindfulness-based interventions can complement medication by addressing negative thinking patterns and building emotional resilience. At Avisa Recovery, we emphasize an integrated treatment approach. Our therapists work alongside prescribing professionals to ensure you receive coordinated, holistic care that meets both your emotional and medical needs. Understanding Concerns About Depression Medication Many people hesitate to start medication for depression due to fears about side effects, dependency, or long-term use. These concerns are valid, but they shouldn’t stop you from seeking help. Antidepressants are not addictive, and for many individuals, medication is a temporary tool that provides stability while deeper work takes place in therapy. Side effects may include sleep disturbances, nausea, or changes in energy levels, but these often subside over time. Your provider will monitor your response and make adjustments as needed to ensure your comfort and safety. Knowing When to Reevaluate Your Treatment Medication for depression is not a one-size-fits-all solution. If you’ve started a prescription but haven’t noticed any improvement, or if your symptoms worsen, talk to your healthcare provider. There are many options available, and it’s normal to need some trial and error to find what works best for you. If you’re ever in crisis, feeling suicidal, or experiencing severe distress, seek immediate help. You can call the National Suicide Prevention Lifeline at 988 or go to your nearest emergency room. Get Help Today at Avisa Recovery At Avisa Recovery in New Jersey, we offer personalized support for individuals seeking medication for depression and comprehensive mental health treatment. Our experienced team of psychiatrists, therapists, and support staff will guide you through every step, from diagnosis to finding the most effective treatment plan for your unique needs. You don’t have to face depression alone. Contact Avisa Recovery today to learn more about our services and take the first step toward healing.
Are Percocet Addictive?
Are Percocet addictive? The answer is yes. Percocet is a powerful and addictive drug, and it can be challenging to recognize the signs of addiction. If you or someone you love is struggling with addiction, seeking help is essential. There are a number of treatment options available, and with the proper support and treatment, recovery is possible. At Next Wind Recovery, clients have access to high-quality addiction treatment designed to support their progress through recovery and toward sobriety. Next Wind Recovery is a top-rated drug rehab in New Jersey. Access your free consultation today to learn more about the recovery programs available at Next Wind Recovery. What Are Percocet? Percocet is a combination of oxycodone and acetaminophen. Together, they work to reduce pain and inflammation. Percocet is prescribed for moderate to severe pain and is effective for both short-term and long-term pain relief. It’s important to note, however, that Percocet is a controlled substance, so patients should only use this medication under the supervision of a medical professional. Next Wind Recovery is a New Jersey outpatient rehab center that can help you overcome addiction. How Does Percocet Affect the Brain and Body? Percocet works by binding to opioid receptors in the brain and spinal cord. When this happens, it blocks pain signals from being transmitted. It also stimulates the release of endorphins, which are natural chemicals in the body that produce a feeling of euphoria. This is one of the reasons why Percocet is so addictive – it creates a feeling of pleasure that many people find hard to resist. Percocet also has an anti-inflammatory effect, which helps reduce pain and swelling. The combination of these two effects makes Percocet an effective pain treatment. However, it’s important to note that Percocet can also be abused and can lead to addiction. Percocet can cause liver damage and respiratory depression, lead to an increase in accidents and injuries, and overdose. Percocet can also increase the likelihood of developing depression, anxiety, and other mental health issues. Side Effects of Percocet Like all medications, Percocet has side effects that can range from mild to severe. The most common side effects include nausea, vomiting, constipation, dizziness, and drowsiness. Other side effects may include confusion, headaches, blurred vision, and irregular heartbeat. It’s important to note that taking Percocet can also increase your risk of developing an addiction, so it’s important to talk to your doctor about the potential dangers. It’s also important to note that the side effects of Percocet can be more severe in certain people. For example, people with liver or kidney disease may experience more severe side effects. It’s also important to note that taking Percocet can interact with other medications, so it’s important to talk to your doctor about any other medications you’re taking before you start taking Percocet. Treatment Options for Percocet Addiction There are a number of treatment options available for Percocet addiction. The most effective treatment is a combination of medication and psychotherapy. Medicines like buprenorphine and methadone can help reduce cravings and withdrawal symptoms, while therapy can help a person identify underlying issues that may be contributing to their addiction. In addition to medication and treatment, support groups can also be helpful. Support groups like Narcotics Anonymous (NA) offer a safe space for people to talk about their struggles with addiction and find support from others who are going through the same thing. Finally, it’s important to remember that recovery is a journey and not always easy. It’s important to be kind to yourself and to take things one day at a time. With the right support and treatment, recovery is possible. Find Percocet Addiction Treatment in New Jersey. Through Next Wind Recovery, clients receive compassionate care designed to support their mental, physical, and emotional well-being. Our holistic treatment approach helps clients heal from traumas and physical addiction to substances. We believe in a combination approach that includes traditional therapies and medication treatments that promote total body wellness and healing. We also offer dual-diagnosis treatment options for clients struggling with anxiety, depression, PTSD, and other mental health disorders. This program combines the necessary mental health treatment for both addiction and mental health disorders, medication management to support mental wellness and therapeutic support that promotes healing and positive growth toward recovery goals. Learn more about the treatment options available at Next Wind Recovery in New Jersey today.
What is SMART Recovery?

When it comes to the next big thing in recovery, many scoff at the ideas that are being thrown around, but SMART addiction programs are the real deal. SMART substance abuse programs aim to set manageable short-term goals that motivate recovery and growth. At Next Wind Recovery in New Jersey, we believe in the power of goal setting in combination with additional treatment designed to support client growth and long-term sobriety. We value equality, growth and development, and compassion, individuality, and community. Next Wind Recovery is a top-rated drug rehab in New Jersey. To learn more about how we use SMART addiction recovery programs at Next Wind Recovery, speak with an expert now. What is SMART Recovery? SMART Recovery is a program designed around the idea of the individual post-addiction. Through the concept of individualized recovery through the development of personal goals, the SMART Recovery program supports individual growth through self-empowerment and self-reliance. SMART Recovery focuses clients on four main principles – Building and Maintaing Motivation, Coping with Urges, Managing Thoughts, Feelings, and Behaviors, and Living a Balanced Life. Through a focus on these areas, clients set goals that are “SMART” – Specific, Measurable, Achievable, Realistic, and Timely. These goals are created and maintained through the course of treatment. What Are the Benefits of SMART Recovery? The benefits of the SMART addiction program are endless. The program’s combination of cognitive behavioral therapies ensures that clients are addressing their mental health and addiction through multiple supportive lenses. Through a series of acronyms, SMART substance abuse programs work to help clients cope with urges, maintain motivation, and live a balanced life. SMART recovery meetings teach individuals how to cope with desires or cravings following withdrawal. By doing so, the program helps clients prevent relapse and shows them how to address their misdirected thoughts, consider the consequences, and develop a more effective way of addressing the concern. The ABCs of SMART works to address urges and when dealing with emotional upsets. DISARM helps individuals manage harmful self-talk and sabotage. By providing these benefits, the SMART program supports client progress and motivation. Another beneficial aspect of the SMART Recovery program is how it helps individuals who are trying to maintain their motivation. By following the program, clients are able to set goals for themselves, but like many others, the motivation to maintain progress towards that goal can be challenging to keep and work for. Through the SMART Recovery tools available, clients develop strategic plans for naming their purpose, creating manageable steps towards achievement, and even naming specific people who can be supportive along each step of the process. Through the creation of this plan, clients can focus on progress and motivation toward their end goal of a more balanced life. Finally, all of this is possible with SMART Recovery, because of the core goal of living a balanced life. SMART addiction programs promote this idea through goal setting and encouraging the ideas of Patience, Practice, Persistence, and Planning. Clients within the SMART Recovery program must learn how to balance their values with their interests and how they can work together to support a balanced lifestyle. Who is SMART Recovery Best For? SMART Recovery is designed so that it can be beneficial in many settings and for many individuals. Through assessment of the needs of the community and feedback from clients, SMART recovery meetings have been designed to support specific client groups like Veterans and First Responders, LGBTQIA+ persons, and Teens/Young Adults. SMART Recovery also offers programs for Friends and Family of those who are addicted or in recovery. How to Find a Rehab That Offers SMART Recovery Treatment SMART Recovery is a cognitive behavioral therapy program designed to empower individuals, build resiliency, and motivate growth toward SMART goals. By calling and asking individualized treatment centers, you can ask whether they offer SMART Recovery programming or check out Next Wind Recovery, our New Jersey treatment facility designed with the individual in mind. At Next Wind Recovery, we offer partial hospitalization, intensive outpatient, outpatient, and aftercare programming for clients who are ready to make a significant change with recovery. Through dual-diagnosis treatment, we support clients with anxiety, depression, and PTSD, in addition to their addiction recovery needs. Next Wind Recovery offers comprehensive addiction treatment programs in New Jersey. To learn more, access your free consultation with a recovery expert at Next Wind Recovery today.
How Does Alcohol Affect the Body?

The body is solid and resilient but can be beaten up, torn down, and rotted from the inside out. Alcohol affects the body by slowing down normal processes. While often minimal, it can be highly damaging in the long run. To learn more about how alcohol affects the body, check us out at Next Wind Recovery. Our comprehensive New Jersey outpatient treatment facility offers support options for those ready for their Next Wind. How Does Alcohol Affect the Body? Alcohol use is so common that many don’t fully comprehend the impact alcohol can have on a person’s body. When an individual drinks alcohol, they will notice some basic reactions to it. They may feel flush, notice their reaction time is slowed, or react differently than expected. These side effects, while common, are only early-onset reactions to the substance. Alcohol is actually a depressant. While some may feel more energetic and lively, and have less stress or social anxiety while drinking, this is a reaction to alcohol’s depression or slowing of functions in the brain. When alcohol affects the body, it delays the ability to process information and reduces the heart rate. This creates a phenomenon for people with high anxiety and stressors where the alcohol seems to bring them to life because they aren’t feeling their typical stress indicators. Is Alcohol Addictive? Alcohol, while safe to consume for adults, can be addictive if not consumed safely. Individuals who over-indulge, binge drink, or drink while using other substances, are at a higher risk of developing an addiction to the substance. Drinking too much too frequently can reduce alcohol’s effects on the body. This is called tolerance, and individuals who develop a tolerance need to drink more alcohol to get the same feeling they did when they first started drinking. While some level of tolerance is acceptable, it is one of the initial warning signs of addiction. Another danger that increases the potential for addiction is binge drinking. Binge drinking is when an individual drinks more than what is considered safe for their gender, body type, and size. This can lead to an overabundance of alcohol in the body’s system. When the body can not process the alcohol fast enough, it can cause individuals to be unable to control their body, lowering reaction time and causing memory loss, known as a “blackout.” Lastly, individuals who drink alcohol while taking another substance are also at higher risk for developing an addiction to alcohol. Because of how alcohol affects the body, combined with another substance, a depressant, or painkiller, this can cause extreme depression in the body’s system. Overdoses with combined substances have been linked to comas, strokes, heart attacks, and death. What Are the Effects of Alcohol Abuse? Individuals who drink alcohol and become addicted to it don’t just have short-term problems to deal with. The effects of alcohol abuse on the body can be a lifelong struggle. Psychologically, individuals may deal with the after-effects of alcohol for the rest of their life. Alcohol addiction can cause depression and anxiety, and can be associated with other diagnosable mental health disorders. Individuals addicted to alcohol experience more major depressive episodes than those who do not. The effects of alcohol abuse are also linked to sleep disorders and suicidal thoughts and tendencies. Alcohol can also be associated with dramatic changes in personality and reactions to stressful situations. The effects of alcohol abuse can have long-term effects on the body as well. Physically, clients have a higher risk of developing certain types of cancer. They are at a higher risk for liver failure because of how alcohol gets filtered out of the blood system. Following alcohol addiction, individuals may get more infections and have more severe illnesses. How to Find Alcohol Addiction Treatment in New Jersey When considering how alcohol affects the body and how to find addiction treatment programs in New Jersey, it is essential to consider the client’s needs and how local therapy in New Jersey can help. Next Wind Recovery, located in Teaneck, NJ, provides supportive outpatient opportunities for clients ready to change their lifestyles. Our medical professionals work with clients through individual and group therapies to help them achieve their sobriety goals. At Next Wind, we realize that with addiction often comes addiction mental health concerns that must be addressed to treat the whole patient. That is why we offer dual diagnosis treatment for our clients. By treating our client’s mental and physical health concerns, they can focus on total mind and body wellness. Learn more about how alcohol affects the body by speaking with a Next Wind Recovery NJ counselor.
What is the Timeline for Heroin Withdrawal?

Identified a century ago as a potentially addictive and dangerous drug, heroin use has continued across the globe. Heroin is often looked at as a gateway drug to harder drugs as it is easy to access and extremely addictive. Many individuals claim that heroin was their first illegal drug use. At Next Wind Recovery, we want to help clients achieve and maintain long-term sobriety. Through this process, we offer comprehensive addiction and mental health care that encourages personal growth and life-long change. Next Wind Recovery is a top-rated drug rehab in New Jersey. Talk with someone from Next Wind Recovery about detoxing from heroin today. What is Heroin? Heroin is a narcotic that relieves pain while creating a calming and euphoric high. Heroin is an extremely effective painkiller with addictive qualities. Heroin, while it has previously been used in medical procedures, was found to be so detrimental to the recovery process of clients that it was made illegal in 1924. This illegal opioid narcotic was the most commonly used illegal painkiller until the introduction of fentanyl in the 1980s. Heroin acts like other common prescription painkillers and is often the first illegal drug that individuals use following problematic use with prescription opioids. Additionally, individuals who use heroin often struggle with other illegal drugs as well, using heroin as a boost because of its’ low cost and how easily they can access it. How Does Heroin Affect the Body? Heroin is a very versatile opioid. Individuals looking for heroin can find it in pill, powder, or liquid form, each producing a slightly different high that impacts the body at various speeds. Individuals who inject heroin with a needle can expect to experience a rushing high with an immediate impact. However, it also wears off more quickly, while individuals who ingest the drug in pill form should expect a longer-lasting high that starts more gradually. When an individual uses heroin, they can expect to feel a calming euphoria connected with pain relief. Heroin blocks the opioid pain receptors in the body, preventing the nerves from identifying pain. In doing so, there is a rush in the brain’s reward center. This rush that creates the calming euphoria is what increases the likelihood of becoming addicted to heroin. Heroin becomes addictive when an individual can not stop using it, chasing the high and pain relief it brings. What are the Symptoms of Heroin Withdrawal? Following heroin addiction, individuals can expect to have some moderate to severe physical, emotional, and mental withdrawal symptoms. Heroin is a drug that impacts the brain and body equally, making the withdrawal process difficult to manage independently. The physical symptoms of heroin withdrawal often include increased pain in the body. Muscle aches, uncontrollable twitching, and joint pain are every day due to overactive nerves. Clients can also expect difficulty sleeping, nausea, weight loss, and diarrhea. However, sometimes the mental and emotional symptoms of heroin withdrawal can be an even more difficult challenge. During the withdrawal period, individuals can expect to experience cravings, depression, anxiety, and mood swings. Heroin has been found to alter the brain’s white matter, changing reactions to stressful situations and decision-making. What is the Timeline for Heroin Withdrawal? The timeline for heroin withdrawal can vary dramatically depending on the support system individuals choose to utilize. Those who attempt to undergo heroin withdrawal independently can expect to experience more severe symptoms with a longer recovery timeline. In contrast, individuals who use a detox center or are medically supervised during withdrawal often experience a shorter and less painful withdrawal due to medications and medical support available throughout the withdrawal process. Typically, individuals begin to feel withdrawal effects in the first 8-16 hours following the last use. Initial symptoms include flu-like symptoms and cravings. Symptoms of withdrawal typically peak in the first 72 hours. At this point, symptoms are the most different for those with support and those going through it independently. Initial withdrawal symptoms can last up to 10 days, but the psychological symptoms of addiction can last for an additional six months. Anxiety, depression, and sleep problems are expected early in rehabilitation treatment and can be more severe if an individual does not utilize treatment. Next Wind Recovery Offers Heroin Addiction Treatment in New Jersey At Next Wind Recovery, we offer intensive outpatient treatment in New Jersey to help clients through the initial stages of withdrawal and addiction treatment. Our New Jersey addiction treatment center offers clients a safe and supportive environment to work through a holistic treatment plan designed to support their physical, mental, and emotional health. Our comprehensive treatment center offers active options with additional aftercare support for individuals who graduate from our treatment programs. What makes us incredibly unique is our different mental health treatment options that individuals can combine with our addiction therapy to provide inclusive treatment options for individuals struggling with mental health diagnoses and addiction. To learn more about heroin addiction treatment at Next Wind Recovery, speak with a counselor today.
